A modern clinic can’t afford “paper-chaos”, clipboards get lost, signatures are hard to verify, and a rushed front desk can accidentally skip the very consent that protects both patient and provider. In 2026, the common approach is simple: collect consent digitally, make it readable on any device, and store it in a way your team can actually find later. This guide breaks down what medical consent is, the three consent levels you’ll see from check-in to emergency care, and the five digital consent forms most clinics rely on today, with practical examples you can borrow.
What is medical consent?
Medical consent is a patient’s permission for a clinician or clinic staff to provide care, share certain information, or take an action related to treatment. It’s an ethical requirement and documents the patient’s decision to proceed. In everyday practice, consent shows up as a quick “yes” at check-in, a detailed signature before a procedure, or a documented plan for future decisions if a patient loses capacity.
If you’re building or updating your paperwork, start with a template library designed for healthcare teams. Although there are countless healthcare form templates, from a birth certificate template to health tracking forms, there are also plenty of medical consent forms. Jotform’s medical consent form templates are a good reference point for common scenarios and digital signing workflows.
The 3 levels of medical consent: From check-in to emergency care
Consent requirements aren’t a one-size-fits-all process. Most clinics work across three levels, everyday permissions, detailed informed consent for higher-risk decisions, and contingency planning for times when the patient can’t speak for themselves.
1. Implied & express consent
Implied consent is permission communicated through a patient’s actions or inaction, for example, rolling up a sleeve for a blood pressure reading, or seeking help in an urgent situation. Express consent is the direct “yes”, verbal or written, you request for routine care like a physical exam, basic treatment, or a standard lab draw. Think of these as the everyday permissions that keep a clinic running smoothly, they’re real consent, just lighter-weight than a full informed consent packet.
2. Informed consent
Informed consent is the detailed and complex agreement used when the patient’s decision depends on understanding meaningful risks, benefits, and alternatives. It can also be important in medical malpractice claims because it documents the relevant information that was disclosed and that the patient chose to proceed voluntarily.
A helpful way to remember informed consent is the four pillars: competence, disclosure, comprehension, and voluntariness.
- Competence: The patient has the capacity to make healthcare decisions (or a legally authorized representative does).
- Disclosure: The clinician shares material information, what the procedure is, why it’s recommended, risks, benefits, and alternatives.
- Comprehension: The patient understands the information, with space for questions and plain-language explanations.
- Voluntariness: The decision is made freely, without coercion, pressure, or unfair influence.
3. Advance directives
Advance directives are the tools that allow patients to set out their treatment preferences in advance, whether through a healthcare proxy, living will, or a DNR form, so those decisions can guide care if a patient is no longer able to give it expressly. You can frame this as “Designating a Surrogate in Advance”, the patient documents instructions for future care before they lose the capacity to communicate, and may name an agent (healthcare proxy) to decide on their behalf. That matters in real life because capacity can change quickly after an accident, during severe illness, or under sedation.
The 5 types of digital consent forms your clinic needs in 2026
If your clinic is still relying on a single “consent to treat” page, you may be missing scenario-specific disclosures that patients (and auditors) expect today. Here are five consent form types that translate especially well to secure digital workflows.
1. HIPAA intake & administrative consent forms
This is the front-desk bundle that covers the “business” side of care, patient intake consent, acknowledgment of privacy practices, billing/insurance permissions, and the basic administrative disclosures your clinic needs to operate. Consent practices increasingly emphasize opt-in consent as an affirmative agreement rather than a passive signature on a clipboard. Consent best practices emphasize opt-in consent as an affirmative, clear agreement, which maps nicely to healthcare intake checkboxes for things like texting appointment reminders or sharing records with a specialist.
What a strong digital intake consent can include:
- A checkbox acknowledging receipt of your privacy notice
- Separate checkboxes for communications (SMS, email, phone)
- A “release to insurer” or billing authorization section
- A signature field plus date/time stamp for auditability
Example: A private practice might let patients opt in to SMS reminders, but keep consent to share PHI with a billing service as a separate, clearly labeled checkbox. Digital forms make that separation obvious, and reduce the chance that staff “assume” consent where it wasn’t given.
2. Surgical & high risk medical consent forms
For surgery and other higher-risk interventions, this is often the most critical consent workflow. These forms should reflect the duty of disclosure, meaning the patient is told the information a reasonable person would consider important before deciding. They also need to document the patient’s right to refuse or defer treatment after hearing the risks and alternatives. In cases where a patient chooses to leave care after those risks have been explained, an against medical advice form can help document that decision.
Why digital matters here isn’t just convenience, it’s readability. Long risk disclosures often get compressed onto photocopied pages, and the result is tiny text, missing initials, or an unreadable carbon copy. A digital surgical consent can:
- Present risks in scannable bullets
- Use required “acknowledge” checkboxes for key points
- Add plain-language prompts (e.g., “Describe the main risk in your own words”)
- Capture e-signatures with consistent formatting and timestamps
Example: For a colonoscopy, you might list sedation risks, perforation risk, and alternatives (watchful waiting, different tests) in short bullets, then require a checkbox that confirms the patient had the chance to ask questions. If you ever need to prove disclosure happened, that structure may provide stronger evidence, more verifiable evidence than a blurry scan.
3. Telehealth & remote care medical consent forms
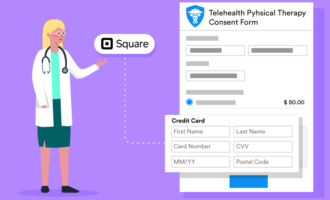
Telehealth consent is often express consent for digital care, but many clinics also provide a more detailed informed consent that mirrors in-office disclosures when the clinical risk is similar. In 2026, your telehealth consent may also benefit from covering “platform security”, patients deserve to know how video/audio data is protected, what to do if their connection fails, and how your clinic handles privacy in a remote setting.
Practical telehealth consent sections typically include:
- Technology limits (what telehealth can and can’t do)
- Emergency plan (what happens if symptoms escalate)
- Privacy expectations (patient should be in a private space when possible)
- Platform security statement (encrypted connection, access controls, vendor agreements as needed)
Add a required checkbox that confirms the patient understands telehealth may limit physical exams, and that they can request an in-person visit if it’s appropriate at any time.
Example: A counseling practice might include a short “backup plan” clause, if video drops, the clinician will call the patient’s phone number on file, and sessions won’t be recorded without separate consent. That’s small, but it prevents confusion when something goes wrong mid-visit.
4. Specialized medical consent for sensitive clinical data & genetic testing
Some data categories are sensitive enough that a blanket signature may not be appropriate or compliant. For HIV testing, substance use treatment information, reproductive health details, or genetic results, clinics often move toward granular consent, separate opt-ins for separate uses, so patients can make informed choices about disclosure and downstream sharing. Genetic testing consent, for example, commonly addresses privacy concerns and implications of results, including who may access the information.
How digital can help with granular consent:
- Separate checkboxes for each sensitive category
- Clear “who gets access” disclosures (lab, specialist, insurer, patient portal)
- Optional consent for research use (when applicable)
- A record of exactly what the patient agreed to, and when
Example: A clinic offering pharmacogenomics might present two separate decisions, consent to run the test, and consent to store results in the patient portal. Patients who want the care benefit but prefer limited sharing can choose accordingly, and your team still gets clean documentation.
5. Contingency & dependent care consents for TPA
Third-Party Authorization (TPA) is often essential for continuity of care when the patient isn’t the only decision-maker, parents consenting for minors, caregivers acting with documented permission, decision-making for surrogates or adult children managing elder care. When an adult lacks capacity, clinicians often rely on an authorized surrogate unless there’s a clearly applicable advance directive.
A solid TPA workflow can include:
- Relationship to patient and authority scope (what decisions or records access is allowed)
- Emergency contact details
- Expiration date or review cadence
- A quick way to present the document to another provider when needed
Example: For a summer camp program, parents might sign a medical authorization allowing a designated counselor to authorize treatment if the parent can’t be reached. For elder care, an adult child might need authorization to discuss medications with a specialist. Either way, having a signed document that’s searchable and shareable can prevent delays.
Meet Jotform’s HIPAA-friendly consent forms
If your goal is to digitize consent and prioritize privacy, Jotform offers HIPAA-friendly forms built for healthcare workflows, including medical consent, intake, and telehealth templates. You can start with a consent template library, customize fields in minutes, and collect e-signatures on mobile so patients can complete paperwork before they arrive.
A few HIPAA-friendly highlights clinics look for:
- HIPAA-focused account features and a BAA (when enabled): Intended to support covered entities in handling PHI with appropriate safeguards.
- Secure signing for consent documents: HIPAA-friendly e-signatures with encryption and digital certification for signed records.
- Healthcare integrations: Send form data into the EHR tool of your choice with healthcare-category integrations.
Skip the manual filing and modernize your clinic with Jotform today
When consent is handled on paper, printing, signing, scanning, then filing, it adds friction for staff and increases compliance risk. With Jotform, you can connect forms to automated steps, route submissions for review, and keep consent records organized in one place.
Here are a few ways clinics modernize fast:
- Turn consent submissions into tasks, route them to the right staff member, and track progress in Jotform Workflows, using the Consent Approval Workflow Template instead of chasing paper.
- Collect consent during scheduling and send automated reminders with Jotform Appointments, so patients arrive prepared, not rushed.
- Start from 100+ ready-made medical consent form templates, then tailor them to your specialty, from telehealth to surgical consent to genetic testing.
The best time to modernize consent is often before the next audit, complaint, or “we can’t find that form” moment. Start with one high-impact workflow, like digital intake plus telehealth consent, then expand to surgical, sensitive-data, and authorization scenarios as your team gets comfortable.
Other types of medical consent forms
This content is for informational purposes only. Jotform is not a law firm and is not providing any legal, financial, or other advice. Please consult a licensed attorney and/or other applicable professionals.
This article is for private practice owners, clinical directors, and medical compliance officers looking to digitize their paper trail while maintaining strict legal and ethical standards.






















































































Send Comment: