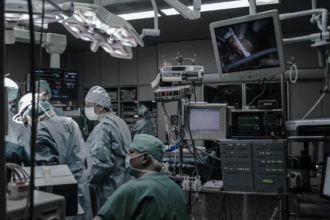
When you think of modern marvels of innovation, the supercomputer may come to mind, with good reason. Computers like the RIKEN MDGRAPE-3 are designed to help us better understand biological molecules and therefore better understand ourselves. While inventions like these deserve praise, there are other innovations with significant impact that often go unnoticed.
Take the electronic health record (EHR), for example. It has had a huge positive impact on society but doesn’t get talked about much. I get it. EHRs aren’t as exciting as making a video call to a colleague halfway across the world, but the technology could save your life one day.
Imagine you get in a car accident in a different state. You’re rushed to a hospital where you’ve never been seen before and no one knows you. How will the staff know about the pain medication you’re deathly allergic to? Thanks to electronic health records, hospital staff will have near-instant access to your medical information, avoiding a potentially deadly mistake.
Sure, that example is dramatic, but the point is that EHRs have drastically improved healthcare. The three key areas of improvement are efficiency, quality, and convenience.
Pro Tip
Expertly collect and organize medical records online with Jotform’s HIPAA-enabled medical forms.
Electronic health records improve day-to-day healthcare
EHRs make the transmission of health data faster than ever. A specialist can request relevant information to make a better diagnosis and efficiently inform your primary doctor of your visit, all by accessing your EHR. And if you’re treated in a different state, country, or even continent, doctors can access your medical history via your EHR and provide you the care you need. They can even consult with your doctors back home.
This doesn’t mean healthcare providers can use this information however they see fit. They must abide by HIPAA laws to protect both their organization and their patients. Let’s look at how HIPAA affects your handling of protected health information.
HIPAA and your organization
HIPAA applies to all organizations, individuals, and agencies that match the description of a covered entity. Covered entities are required by law to protect an individual’s rights when handling their protected health information (PHI). They’re also required to enter a business associate agreement (BAA) with anyone who will have access to PHI.
How can you determine if you’re a covered entity? The U.S. Department of Health & Human Services website has a helpful table for checking your status. In short, if you’re a healthcare provider, a health plan, or a healthcare clearinghouse, you’re likely a covered entity.
But what if you know that you’re subject to HIPAA regulations and already use compliant software?
Does my organization enable HIPAA compliance just because my EHR software is HIPAA-enabled?
The answer is, it depends. Having HIPAA-enabled EHR software doesn’t mean your organization operates in a compliant way. Misusing or mishandling compliant software can open you up to security and privacy breaches. With that in mind, you need to cover all of your bases.
Start by reviewing the workflow for patient information. For example, how does your staff collect, store, and share patient information? If you’re gathering patient information electronically, are those forms HIPAA-enabled? Clearly, organizations that want to respect patient privacy need to look at how their employees work as a whole and not just at specific components of HIPAA compliance.
HIPAA compliance is more than just signing a business associate agreement
To ensure your organization is fully compliant and protected, you have to do more than just sign a contract. Your organization’s leadership must appoint privacy and security officers who will be responsible for developing, documenting, and maintaining practices that help your organization enable HIPAA compliance. These security leaders are also responsible for promoting and emphasizing the importance of security within the organization.
One of the more challenging duties of the security and privacy officer is maintaining compliance. This maintenance requires regular communication with staff to accomplish three objectives:
- Make sure everyone understands their role in keeping your practice compliant.
- Communicate what’s expected of employees when they handle PHI.
- Regularly communicate changes and ensure that staff put into practice your privacy and security policies.
The responsibilities of this role can seem daunting, but keeping your organization and patients secure has lasting positive effects.
Protecting your patients protects your reputation
Electronic health records make better patient care possible, but they aren’t without risk. Proactive organizations can mitigate that risk. Take your patients’ privacy and security seriously, and you’ll build the trust of your patients and the reputation of your practice.




























































































Send Comment: