Medical error is the third leading cause of death in the U.S. An error can be made in planning patient care, in failing to follow the plan, or because the healthcare professional didn’t have all the information necessary to treat the patient. One of the most effective strategies for avoiding medical errors is gathering accurate patient data and making the patient a partner in their care.
You can collect patient data in several different ways — by conducting an interview in a clinical setting, by having the patient complete a paper form, or by having the patient fill out an online form. There are pros and cons to each method.
Here are five patient data-collection best practices healthcare providers should follow.
5 patient data-collection best practices
- Always be transparent
- Digitize data collection as much as possible
- Use HIPAA-enabled solutions
- Be thorough when requesting data
- Consider using customized forms
1. Always be transparent
The most important part of patient data collection is the patient’s cooperation. But patients cannot be expected to cooperate unless providers are fully transparent about why their data is being collected. They need to know what their data will be used for and where and how it will be stored.
The best assurance for patients is when you provide them with your practices that help with Health Insurance Portability and Accountability Act (HIPAA) compliance as well as any unique data storage practices. Take the time to answer patient questions and explain how providing this information can help you treat them.
2. Digitize data collection as much as possible
Paper files can be misplaced, can’t be accessed from multiple locations, and have to be physically moved when the patient sees another healthcare provider who needs their information. This can create information gaps.
What if a hospital doesn’t have the most recently updated list of the patient’s medications? Collecting information digitally ensures that this information is in the patient’s record and that it can be easily transmitted and cross-referenced.
Some providers have tried to go digital by scanning paper files. However, this often just creates an image of the form that can’t be searched. Additionally, because it’s an image of the patient’s handwriting, you may not be able to decipher it. It’s best, whenever possible, to start the process with electronic records.
3. Use HIPAA-enabled solutions
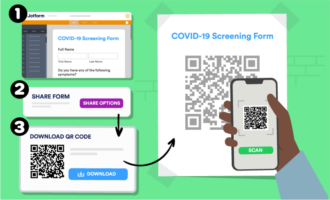
If you’re collecting data directly from the patient, it’s essential to use a HIPAA-enabled web form like those provided by JotForm. There may be cases when paper is necessary, like providing a printout of your patient data-collection policies, but you can cut down on your paper usage and increase efficiency by using online forms.
Always use secure forms from a provider that has signed a business associate agreement (BAA). This protects you if they disclose protected information.
In addition, using a web form eliminates the likelihood that the person inputting the patient’s data from a paper form can’t read their handwriting or mistypes it. Paper forms may also end up in the wrong hands or filed in the wrong place, which could lead to a HIPAA breach.
4. Be thorough when requesting data
Patient intake forms are an excellent opportunity to collect your patient’s health history, but so are regular follow-up forms. Insurance information, contact information, current medications, health history, and a checklist of symptoms are all a basic start. It’s good to conclude by asking the patient if there’s anything else you should know.
Sending patients an online form to fill out prior to their initial office visit allows them to look up their health history and medications. For example, they might not know the dosage of their blood pressure medication off the top of their head, but when they’re at home filling out the form, they can check the bottle in their medicine cabinet.
5. Consider using customized forms
If your practice treats patients with different conditions, you should create forms tailored for them. For instance, ask your diabetic patients about their hospital admissions, diet, and if they’re interested in education to help them manage their condition.
A customized form improves the patient experience while providing you with relevant information for the patient’s treatment. You can give a patient better information if you know, for example, that they’ve been hospitalized with low blood sugar in the past six months and want education on diabetes management.
The information you collect from your patients will help you treat them and could ultimately prevent an error from occurring if they’re seen by someone else. Be thorough in your data-collection practices, and use HIPAA-enabled solutions to provide them with the best possible care.
Photo by Tima Miroshnichenko






















































































Send Comment:
1 Comment:
April 15, 2023
Debitis commodo fugi